Understanding Continuous Glucose Monitoring
From professional athletes perfecting peak performance to millions managing diabetes in 2026, continuous glucose monitoring (CGM) is transforming how Americans track blood sugar. Discover how CGM tech is changing healthcare, daily life, and personal wellness across the United States.
What Is Continuous Glucose Monitoring?
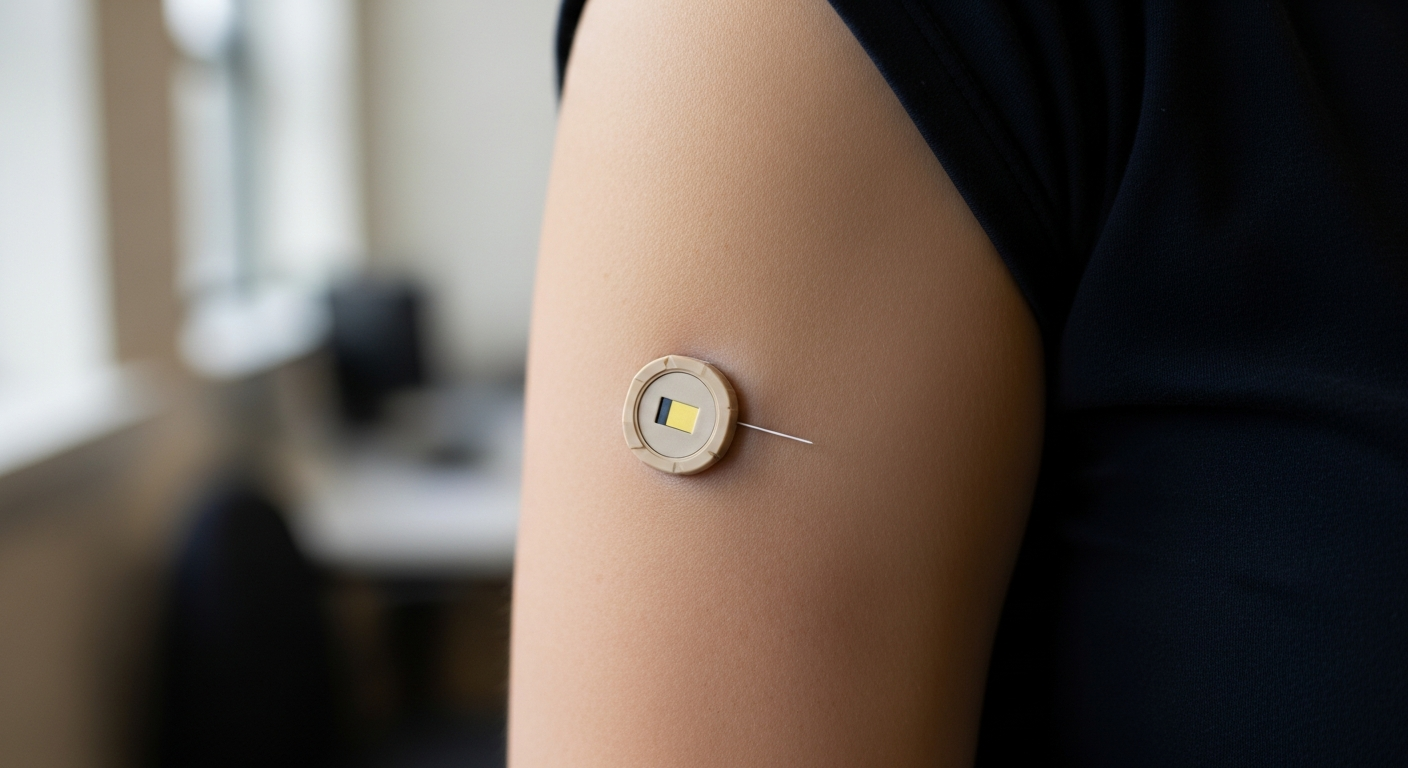
Continuous glucose monitoring involves wearing a small sensor device that measures glucose levels in tissue fluid beneath the skin. The sensor transmits data wirelessly to a receiver, smartphone app, or insulin pump, providing glucose readings every few minutes. This technology eliminates the need for frequent finger pricks while offering comprehensive glucose pattern information that helps users understand how food, exercise, stress, and medications affect their blood sugar levels.
Modern CGM systems consist of three main components: a disposable sensor worn on the skin, a transmitter that sends data, and a display device or smartphone app. The sensor typically requires replacement every 10-14 days, depending on the specific model and manufacturer specifications.
How CGMs Are Used in American Healthcare
Healthcare providers across the United States increasingly recommend CGM technology for patients with Type 1 and Type 2 diabetes. Endocrinologists and primary care physicians use CGM data to make more informed treatment decisions, adjusting insulin dosages and medication regimens based on detailed glucose patterns rather than isolated readings.
Many American hospitals and clinics have integrated CGM data into electronic health records, allowing healthcare teams to review glucose trends between appointments. This integration enables more personalized diabetes management plans and helps identify patterns that might otherwise go unnoticed with traditional monitoring methods.
The technology also supports telemedicine consultations, particularly valuable in rural areas where specialist access may be limited. Patients can share their glucose data remotely, enabling healthcare providers to make timely adjustments to treatment plans without requiring in-person visits.
Benefits for Diabetes Management in the U.S.
CGM technology offers numerous advantages for diabetes management in the American healthcare context. Users report improved quality of life due to reduced anxiety about glucose levels and fewer disruptions from finger stick testing. The devices provide alerts for impending high or low glucose episodes, potentially preventing dangerous situations.
Studies conducted in American medical centers demonstrate that CGM users often achieve better glycemic control, with improvements in hemoglobin A1C levels. The technology particularly benefits individuals with frequent hypoglycemic episodes or those who experience hypoglycemia unawareness.
For parents of children with diabetes, CGM systems provide peace of mind through remote monitoring capabilities. Many devices allow family members to receive glucose alerts on their smartphones, enabling them to assist with diabetes management even when physically separated.
Insurance Coverage Considerations
Insurance coverage for CGM devices varies significantly across different plans and providers in the United States. Medicare covers CGM systems for beneficiaries who meet specific criteria, including frequent blood glucose testing requirements and insulin use. Most major private insurance companies also provide coverage, though prior authorization may be required.
Medicaid coverage varies by state, with some states providing comprehensive CGM coverage while others have more restrictive policies. Patients should verify their specific coverage details with their insurance providers, as copayments and deductibles can affect out-of-pocket costs substantially.
Many manufacturers offer patient assistance programs to help reduce costs for individuals with limited insurance coverage or high deductibles. These programs can significantly lower the financial barrier to accessing CGM technology.
Cost Analysis and Provider Comparison
The financial investment in CGM technology includes both initial device costs and ongoing sensor replacement expenses. Understanding these costs helps patients make informed decisions about diabetes management options.
| Provider | Device Cost | Monthly Sensor Cost | Insurance Coverage |
|---|---|---|---|
| Dexcom | $300-400 | $250-350 | Medicare/Most Private |
| Abbott FreeStyle | $200-300 | $150-200 | Medicare/Most Private |
| Medtronic | $400-500 | $300-400 | Medicare/Most Private |
| Senseonics | $1,000-1,500 | $200-250 | Limited Coverage |
Prices, rates, or cost estimates mentioned in this article are based on the latest available information but may change over time. Independent research is advised before making financial decisions.
Making the Decision
Choosing to use CGM technology involves considering personal lifestyle factors, diabetes management goals, and financial circumstances. Healthcare providers can help evaluate whether CGM technology aligns with individual needs and treatment objectives.
Many patients find the transition to CGM monitoring requires an adjustment period as they learn to interpret continuous data rather than single point-in-time readings. Support from diabetes educators and healthcare teams proves valuable during this transition phase.
Continuous glucose monitoring represents a transformative tool in modern diabetes care, offering unprecedented insights into glucose patterns and enabling more precise management strategies. As technology continues advancing and costs potentially decrease, CGM systems may become even more accessible to the broader diabetes community in the United States.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.