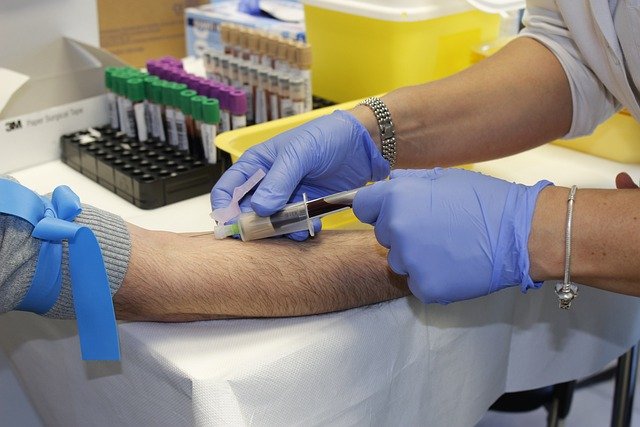
HIV Symptoms And Early Warning Signs 2026
Early detection of HIV makes a crucial difference in health outcomes, especially in the United States, where access to modern treatment and awareness is key. Know the subtle early warning signs of HIV in 2026, from flu-like symptoms to skin changes, and protect both yourself and your community.
Many people think HIV always causes obvious symptoms right away, but early infection can be subtle or feel like a short-lived flu. Because these signs are not specific to HIV, the most reliable way to know your status is timely testing with an appropriate test type. Understanding common early patterns can still be useful for deciding when to seek care—especially after a potential exposure.
Recognizing Common Early HIV Symptoms in 2026
Early HIV symptoms most often refer to acute HIV infection, which can occur after the virus enters the body and begins to replicate. Some people notice symptoms, while others do not. When symptoms do occur, they commonly include fever, chills, sore throat, headache, muscle or joint aches, swollen lymph nodes (often in the neck), rash, and pronounced fatigue. Some also report night sweats, mouth ulcers, or gastrointestinal symptoms like nausea or diarrhea.
A key challenge is that these signs overlap with many other illnesses, including seasonal respiratory viruses and mono-like infections. Symptom severity varies widely, and the absence of symptoms does not rule out infection. If you associate symptoms with a recent potential exposure, it can be helpful to share that timing with a clinician because it may influence which test is most accurate.
Differences in HIV Signs Across Age Groups
Age can influence how symptoms are noticed, described, or attributed. Adolescents and young adults may dismiss fever, sore throat, or rash as a routine illness, and they may be less likely to seek medical care quickly. In adults balancing work and family responsibilities, fatigue and body aches may be written off as stress or lack of sleep. Older adults may experience more complex health baselines, where new symptoms are mistakenly attributed to aging or other chronic conditions.
It is also important to separate early symptoms from later-stage concerns. HIV can be present for years without noticeable symptoms, and when symptoms occur later, they can reflect immune system strain and opportunistic infections. Because symptom patterns are not a dependable way to identify HIV, age-specific differences mainly affect how quickly someone pursues testing and how clinicians consider HIV in the differential diagnosis.
When to Seek Testing and Medical Care
Testing is recommended after a potential exposure even if you feel well. Seek prompt medical care if you have symptoms that concern you and you’ve had a recent risk exposure such as condomless sex, a condom break, sharing injection equipment, or a sexual partner with unknown status. Clinical care is also important if you believe you need post-exposure prophylaxis (PEP), which is time-sensitive and generally needs to be started as soon as possible after exposure.
Different tests detect infection at different points in time. Many clinics use lab-based antigen/antibody tests, which can detect infection earlier than antibody-only tests. Nucleic acid tests (NAT) can detect infection earlier still in some situations, but availability and clinical use vary. If an initial test is negative soon after exposure, clinicians may recommend repeat testing after a specific interval to account for the window period.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
Impact of Social Stigma on Early Detection
Stigma can delay testing and care even when symptoms are present. People may worry about judgment from family, peers, or healthcare staff; fear confidentiality breaches; or avoid care due to shame related to sex, sexual orientation, drug use, or relationship dynamics. This can lead to missed opportunities for early diagnosis and for prevention steps that protect partners.
Reducing stigma often comes down to practical, supportive choices. Many communities offer confidential testing options through local services, public health clinics, and community health centers. Some people prefer discussing sexual health with a clinician who is experienced in nonjudgmental care. If cost or privacy concerns are a barrier, asking about sliding-scale clinics, confidential billing practices, or community-based programs can help people access testing sooner.
Advances in HIV Prevention and Awareness in the U.S.
In the mid-2020s, HIV prevention and awareness in the United States increasingly focus on pairing education with practical tools. Pre-exposure prophylaxis (PrEP) is a well-established prevention strategy for people at ongoing risk, and post-exposure prophylaxis (PEP) remains an important emergency option after a possible exposure. Public health messaging also emphasizes the importance of routine screening as part of sexual health, because relying on symptoms alone misses many infections.
Awareness efforts also highlight that effective medical treatment can reduce the amount of virus in the body to very low levels. When a person maintains an undetectable viral load as confirmed by clinical testing, the risk of sexual transmission is effectively eliminated according to the U=U framework (Undetectable = Untransmittable). This does not remove the need for medical follow-up, adherence support, or sexually transmitted infection (STI) screening, but it can reduce fear and misinformation and encourage earlier engagement with healthcare.
Recognizing possible early HIV symptoms can help people decide when to test, but symptoms alone cannot confirm or rule out infection. Because early signs overlap with many routine illnesses and because HIV can be symptom-free for long periods, timely, appropriate testing remains the most reliable next step after a potential exposure. Approaching testing as routine healthcare—supported by confidential local services and evidence-based prevention options—can reduce delays and improve early detection.