Titanium Frameworks In Dental Implants
From Hollywood smiles to everyday confidence, dental implants using titanium frameworks are setting the standard for lasting oral health in the U.S. in 2026. Discover why American dentists and patients trust titanium for durability, compatibility, and remarkable cosmetic results.
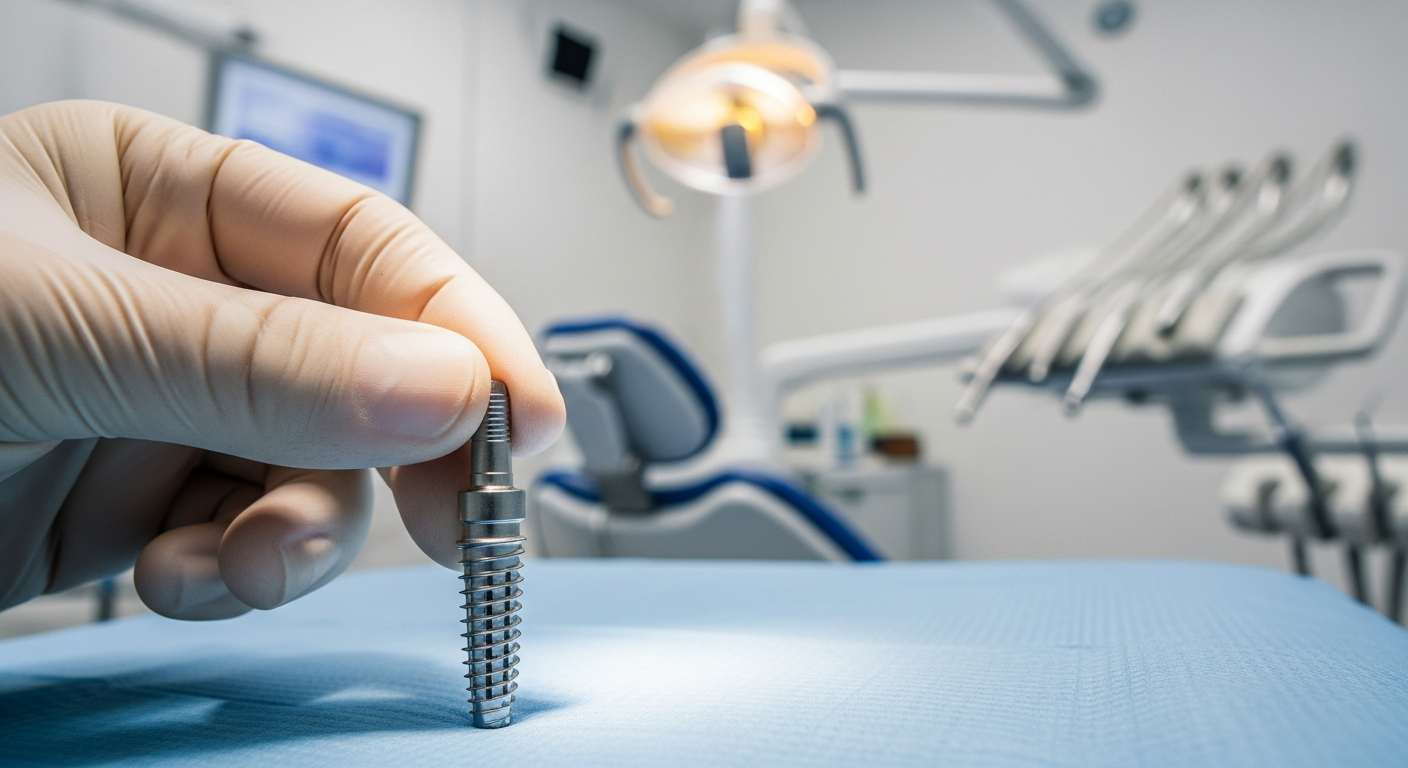
Replacing a missing tooth often requires a material that can handle moisture, pressure, and constant temperature changes while still integrating with living bone. In many implant systems used across the United States, titanium serves as the core structural metal because it balances strength with biocompatibility and has a long clinical track record.
The science behind titanium in dentistry
Titanium’s key advantage is its ability to form a stable oxide layer on its surface when exposed to oxygen. In the mouth, that thin titanium-oxide layer helps protect the underlying metal from corrosion and supports a biological response that encourages bone cells to attach and remodel around the implant surface. Clinically, this bone-to-implant connection is called osseointegration. Modern implant surfaces are also engineered at micro- and nano-scales (through methods such as grit-blasting, acid-etching, or other proprietary treatments) to encourage faster and more consistent early healing.
Long-term benefits and durability
From a functional perspective, titanium frameworks are valued for fatigue resistance: chewing creates repeated loading cycles, and implants must tolerate years of daily forces without deformation. Titanium’s strength-to-weight ratio helps keep components slim while still durable, which can be useful in tight spaces or when restoring multiple teeth. Long-term success also depends on factors beyond the metal itself, including bone quality, implant position, bite forces, oral hygiene, smoking status, and ongoing maintenance. In real-world settings, the durability people associate with titanium is usually the result of a well-planned system: stable bone support, appropriate prosthetic design, and consistent follow-up to manage gum inflammation and bite-related overload.
Titanium implant safety and allergies
Titanium is widely described as biocompatible, meaning it generally performs well in contact with human tissues. True allergy to titanium is considered uncommon, but patient concerns are understandable—especially for individuals with histories of reactions to metals, jewelry, or orthopedic hardware. It is also important to separate different issues that can be confused as “allergy,” such as sensitivity to other metals (for example, nickel, which is not a standard component of commercially pure titanium implants), irritation from plaque-related inflammation, or reactions to dental materials used elsewhere in the restoration.
If a patient has a complex allergy history or prior implant complications, a clinician may discuss options such as alternative materials, component selection (implant, abutment, crown), and documentation of material composition from the manufacturer. In some situations, referral to an allergist or dermatologist for evaluation may be considered, but testing approaches and interpretation can vary.
Comparing titanium to other implant materials
Titanium is not the only option. Zirconia (a ceramic) is used in some implant systems and is often discussed for patients who prefer metal-free restorations. Material choice can affect how components are designed, how they handle stress, and how flexible the restorative plan can be. Titanium systems have a wide range of component options and long-term data across many clinical scenarios. Zirconia implants can offer esthetic advantages in certain thin-gum situations because the underlying material is tooth-colored, but they may have different design constraints depending on the system and case.
Clinicians in the U.S. commonly work with established implant manufacturers, and the “material” decision may also include proprietary titanium alloys designed to improve strength.
| Product/Service Name | Provider | Key Features | Cost Estimation (if applicable) |
|---|---|---|---|
| Titanium implant systems (various lines) | Nobel Biocare | Broad restorative ecosystem; long history of titanium implant use | Typically bundled into total implant fee; varies by clinic and case |
| Titanium implant systems (e.g., Astra Tech Implant System) | Dentsply Sirona | Titanium implant line with platform-specific components and restorative options | Typically bundled into total implant fee; varies by clinic and case |
| Titanium implant systems (e.g., Tapered Screw-Vent) | Zimmer Biomet | Titanium implant designs with multiple diameter/length options | Typically bundled into total implant fee; varies by clinic and case |
| Titanium implant systems | Straumann | Titanium-based systems; some lines include proprietary alloy options | Typically bundled into total implant fee; varies by clinic and case |
| Titanium-zirconium alloy implants (e.g., Roxolid) | Straumann | Alloy designed to increase strength compared with commercially pure titanium | Often similar overall pricing category; varies by clinic and components |
| Zirconia (ceramic) implant systems (metal-free) | Straumann (PURE Ceramic) | Ceramic implant option aimed at metal-free preferences; case selection matters | Components may be priced differently; varies by clinic and lab |
| Zirconia (ceramic) implant systems (metal-free) | Z-Systems | Zirconia implant-focused system; restorative options depend on line | Components may be priced differently; varies by clinic and lab |
Prices, rates, or cost estimates mentioned in this article are based on the latest available information but may change over time. Independent research is advised before making financial decisions.
Advances in U.S. dental implant technology
In the United States, advances in dental implant technology are often less about changing the base metal and more about improving precision, predictability, and patient-specific planning. Digital workflows commonly include 3D imaging, virtual implant planning, and guided surgery tools that help translate a plan into accurate placement. Surface engineering has also evolved, with manufacturers refining implant textures and chemistry to support early stability—particularly useful in immediate placement or shorter healing timelines when clinically appropriate.
Prosthetic materials have advanced as well. Many restorations now pair titanium implants with abutments and crowns designed using CAD/CAM processes, allowing for more consistent fit and contour. These changes can influence comfort, cleanability, and long-term gum health, even though they are not always visible to patients.
Choosing between titanium and other materials is ultimately case-dependent: anatomy, gum thickness, bite forces, esthetic goals, medical history, and clinician experience all matter. Titanium frameworks remain common because they are mechanically reliable and generally well tolerated, while alternative materials may be considered for specific clinical or preference-driven reasons. This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.