Understanding Photo-Biomodulation Benefits
From NBA athletes seeking faster recovery to the latest trends in wellness, photo-biomodulation is gaining traction across the United States in 2026. This innovative light therapy is noted for its potential to help with chronic pain management, enhance energy levels, and support skin health, though individual results may vary and further research is needed to fully understand its efficacy and benefits.
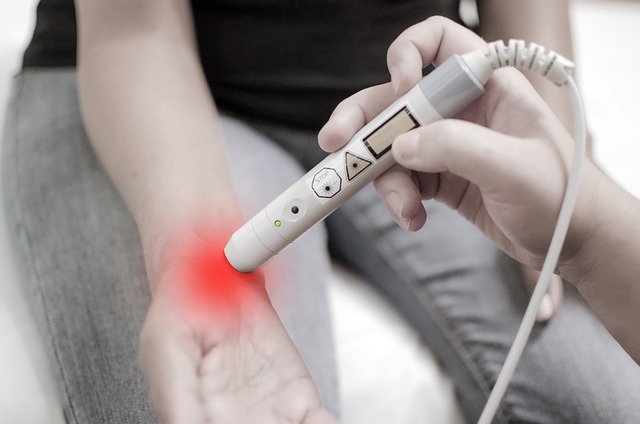
Photobiomodulation uses non‑ablative light to influence cellular activity without the tissue removal associated with cosmetic resurfacing lasers. In skin care settings, it is positioned as a gentle, adjunctive approach that may support recovery and general skin wellness while avoiding downtime. In rehabilitation settings, it is explored for temporary pain relief and improved function when paired with standard care.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
How does PBM work day to day?
Photobiomodulation delivers red and near‑infrared light to tissues at doses designed to trigger a biological response rather than create heat damage. At the cellular level, photons can be absorbed by chromophores such as cytochrome c oxidase in mitochondria, which may influence ATP production and signaling pathways related to oxidative stress and inflammation. In everyday life, that can translate to short, regular sessions targeting the face, joints, or muscles using panels, handhelds, or in‑clinic devices.
In skin contexts, routine use may help calm temporary redness and support normal circulation. In musculoskeletal contexts, steady and consistent dosing protocols are emphasized because many benefits appear to be cumulative. Daily or several‑times‑per‑week sessions are common for home routines, while clinics often schedule a series across several weeks, then reduce frequency as goals are met.
Research and FDA views in the U.S.
The research base for photobiomodulation spans dermatology, dentistry, sports medicine, and pain management. Findings generally suggest potential for temporary pain reduction, improved function in certain musculoskeletal conditions, and support for wound healing and oral mucositis in specific contexts. Evidence quality varies by indication, study design, wavelength, and dose; results are not uniform across all conditions or devices, and protocols are still being refined.
In the United States, some devices are cleared by the FDA for indications such as temporary relief of minor muscle and joint pain, muscle spasm relaxation, and increased local blood circulation. Many consumer products are listed or registered but not specifically cleared for treating diseases. FDA registration does not equal approval or endorsement for a particular medical claim. When considering skin rejuvenation or performance claims, review the exact cleared indications for a given device and discuss expectations with a qualified clinician.
PBM for chronic pain and recovery
For chronic pain, photobiomodulation has been studied in knee osteoarthritis, neck and low back discomfort, and tendinopathies. Some patients report short‑term relief and improved range of motion, especially when PBM is integrated with exercise therapy and standard care. In sports recovery, protocols aim to reduce perceived soreness and support return to activity after training. Outcomes are variable and depend on dose, timing, and individual response.
Photobiomodulation is not a cure for chronic conditions. Rather, it is considered an adjunct that may help manage symptoms and support function. People with complex pain should work with healthcare professionals who can tailor a plan that includes movement, load management, sleep, and nutrition alongside any light‑based therapies.
Home devices vs. pro treatments in the U.S.
Home devices typically use LEDs in red and near‑infrared bands, covering larger areas with moderate irradiance for set durations. They offer convenience, lower per‑session cost over time, and the ability to keep a routine. The trade‑offs include limited professional assessment, variable dosing accuracy, and potential inconsistency if habits slip.
Professional treatments in clinics may use higher‑power lasers or advanced LED systems with targeted applicators, standardized protocols, and therapist oversight. Sessions are usually shorter but more concentrated, and the clinician can adjust parameters based on response. For people pursuing cosmetic laser skin procedures, non‑ablative photobiomodulation is distinct and is sometimes used as a supportive measure for comfort and appearance between higher‑intensity treatments, based on clinician guidance.
Safety and insurance considerations
Safety basics include eye protection for both user and bystanders, respecting device distance and time guidelines, and monitoring skin response. People with photosensitivity, active skin infections, or a history of seizures triggered by light should consult a clinician before use. Caution is generally advised over the thyroid, over active malignancies, and during pregnancy due to limited evidence; professional guidance is prudent. Mild, transient redness or warmth can occur, especially with higher‑power devices.
Insurance coverage in the United States is variable and often limited. Some clinics may obtain coverage when PBM is part of a physical therapy plan for a covered diagnosis, but many plans consider it investigational. Medicare policies are typically restrictive. Health savings or flexible spending accounts may reimburse clinic sessions or certain devices with supporting documentation, such as a letter of medical necessity. Always confirm details with your plan administrator.
Typical costs and comparisons in the U.S. market vary by device class and setting. Single in‑clinic sessions often range from about 30 to 150 dollars, with package discounts for multi‑visit plans. Home LED panels can start near a few hundred dollars and extend beyond 1,500 dollars for larger units. Handheld or professional‑leaning consumer lasers can range from roughly 500 to over 2,000 dollars. Prices differ by region, vendor, and specifications.
| Product or Service | Provider | Key Features | Cost Estimation |
|---|---|---|---|
| Joovv Go portable panel | Joovv | Compact red and near‑infrared LED unit for targeted use | 400–700 USD |
| BIOMAX 600 panel | PlatinumLED | Modular panel with mixed red and near‑infrared LEDs | 800–1,100 USD |
| MitoPRO 1500 panel | Mito Red Light | Large panel offering multiple red and near‑infrared bands | 1,000–1,400 USD |
| LightForce laser session | LightForce used in clinics | Clinician‑delivered Class IV therapeutic laser | 50–120 USD per session |
| K‑Laser therapy session | K‑Laser used in clinics | Targeted Class IV laser protocols in rehabilitation settings | 45–100 USD per session |
| Multi Radiance laser session | Multi Radiance used in clinics | Super‑pulsed laser with LED combinations | 40–90 USD per session |
| THOR PBM session | THOR used in clinics | Professional photobiomodulation protocols with probes or LED clusters | 40–100 USD per session |
Prices, rates, or cost estimates mentioned in this article are based on the latest available information but may change over time. Independent research is advised before making financial decisions.
In summary, photobiomodulation is a non‑ablative light approach that may support skin wellness, temporary pain relief, and recovery when applied with appropriate dosing and expectations. Evidence continues to evolve, FDA clearances are indication‑specific, and outcomes vary across individuals and devices. Deciding between home and professional options hinges on goals, budget, and the value of clinician guidance. Careful attention to safety and a clear understanding of coverage and costs help set realistic, sustainable plans in your area.