The Mechanics of Screwless Dental Implants: Structural Innovations in Restoration
Screwless implant restoration depends on precise engineering rather than a visible fastening bolt. Tapered interfaces, controlled friction, and surface design work together to stabilise components, limit micromovement, and support bone healing when the case and technique are suitable.
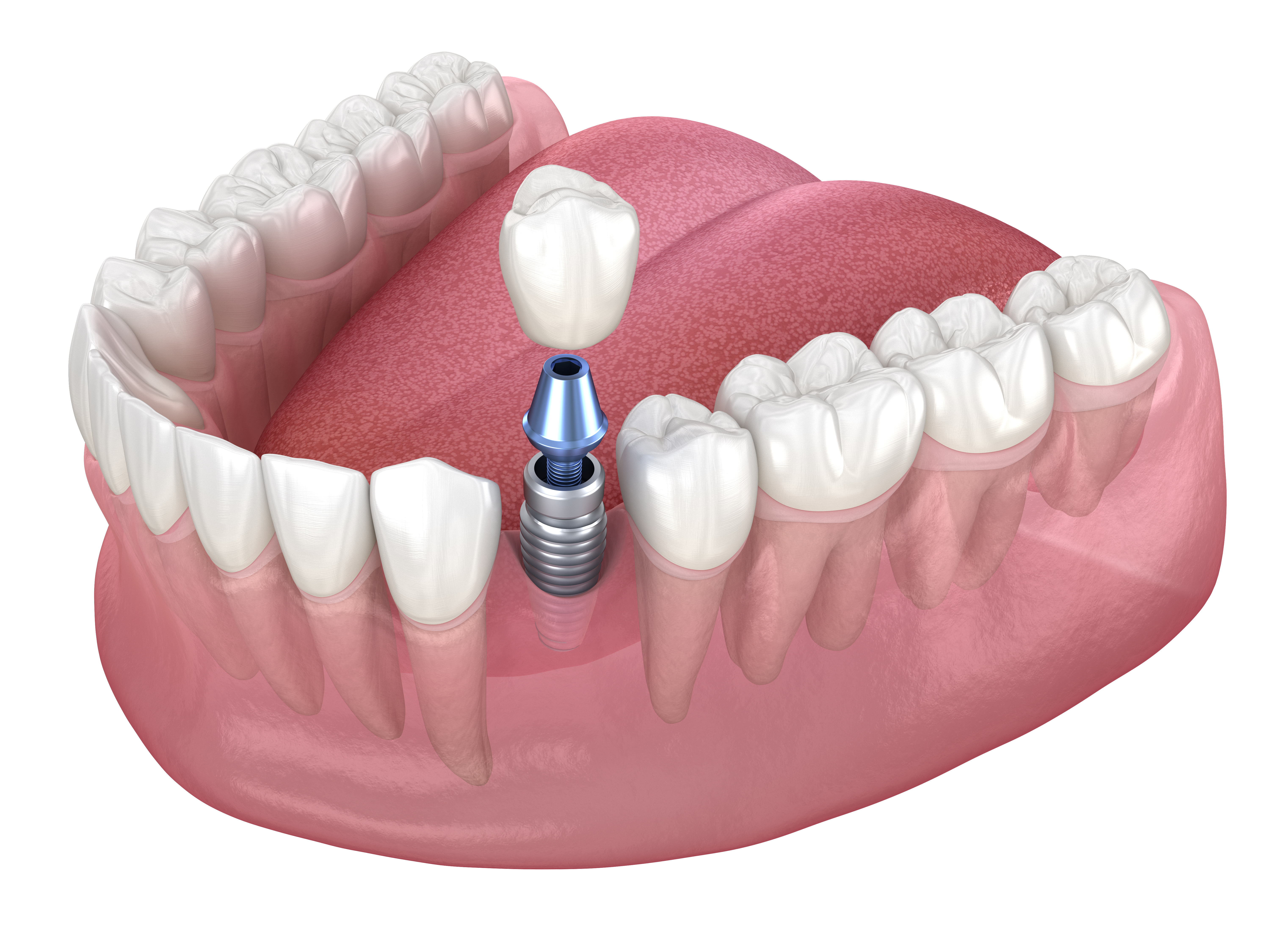
Modern implant dentistry increasingly uses “screwless” concepts to hold a restoration in place—usually by relying on precision-machined taper connections and controlled friction rather than a visible screw-access channel in the crown. It’s important to clarify the mechanics: the implant fixture in bone may still be placed with conventional instruments, but the final abutment–implant and crown–abutment retention can be achieved through press-fit and friction-fit engineering. Understanding how these designs work helps set realistic expectations about stability, maintenance, and long-term serviceability.
A screwless system typically combines (1) a conical or tapered implant–abutment interface, (2) tight manufacturing tolerances, and (3) a restorative workflow that prioritises accurate seating and controlled insertion forces. When these elements align, the connection can behave as a highly stable joint that limits micro-movement, helps seal the implant platform area, and keeps the visible crown free of screw-access holes. When they do not align—because of material wear, contamination, or misfit—retention and retrievability can become more challenging than in screw-retained designs.
How does friction-fit hold a prosthetic?
Friction-fit retention is most commonly achieved using a conical “Morse taper” style connection between the implant and abutment (or between the abutment and a secondary component). As the tapered parts are seated, the contact pressure increases along the cone, generating friction that resists pulling forces and rotational forces. With sufficiently accurate machining and a clean, dry interface, the taper can create a phenomenon often described as a mechanical lock, where removal requires a dedicated disengagement tool or a controlled counter-force.
From a structural viewpoint, the taper’s geometry matters as much as the surface finish. A smaller taper angle generally increases wedging action and resistance to separation, while a longer engagement length can distribute forces over more surface area. This distribution is relevant in chewing because occlusal loads are not purely vertical; they include lateral and oblique components that can promote micro-movement. A stable friction-fit connection aims to reduce that micro-movement, which may help limit fretting and the “pumping” effect that can draw fluids and bacteria at the microgap.
In clinical terms, friction-fit retention can be paired with different crown strategies. Some screwless workflows still use a screw internally to secure an abutment, but the visible crown is cemented or clipped on. Other workflows use fully friction-based retention for the abutment itself. Each approach affects maintenance: cemented crowns can look seamless but carry a known risk of excess cement if not carefully managed; friction-locked components can be secure but may require specific tools and techniques for retrieval.
What changes in press-fit design?
Press-fit (also described as interference-fit) depends on components being manufactured so that, at rest, one part is microscopically larger than the receiving space. When pressed together, elastic deformation and surface contact pressure create retention. In implant restoration, this can show up as friction-locked abutments, coping-to-abutment interfaces, or secondary components designed to “snap” or press onto a base.
Several design changes have shaped modern press-fit behaviour. First, improved CNC machining and quality control allow tighter tolerances, which is essential because retention and stability can be very sensitive to small dimensional differences. Second, connection designs increasingly manage load transfer by controlling where stresses concentrate. Features such as platform switching (where the abutment is slightly narrower than the implant platform) aim to shift the implant–abutment junction inward, potentially influencing stress distribution and soft-tissue behaviour.
Another change is how manufacturers try to minimise rotational play. Anti-rotation features—often internal hexes, splines, or proprietary indexing—can work alongside a taper so the joint resists twisting and lateral forces. For a screwless concept, limiting rotation is critical because even small rotational movement can loosen friction-fit retention over time. Material pairing also matters: titanium-to-titanium interfaces can behave differently from titanium-to-zirconia in terms of friction, wear patterns, and the risk of surface damage during repeated insertion and removal.
Finally, press-fit designs require careful attention to clinical handling. Blood, saliva, or debris at the interface can reduce seating accuracy and change friction behaviour. Seating force must be controlled: too little may leave a component partially engaged; too much may risk damage to the interface or complicate later removal. For Australian clinics, where follow-up intervals and access can vary (metro vs regional), predictable retrievability can be a practical consideration when selecting a restoration design.
How do bioactive surfaces aid integration?
While “screwless” mechanics focus on the prosthetic joint, long-term success still depends on integration between the implant surface and bone. Bioactive or bioenhanced surfaces are engineered to encourage faster or more robust osseointegration by influencing early cell attachment, blood protein adsorption, and the formation of new bone at the interface.
Many widely used implant surfaces are not truly bioactive in the strict chemical sense, but they are bioactive in effect because they are micro-roughened or chemically modified to improve biological response. Examples include sandblasted/acid-etched titanium, anodised surfaces that change oxide thickness and texture, and hydrophilic surface treatments intended to improve wettability. The practical outcome clinicians look for is strong secondary stability over time—bone remodelling and maturation that helps the implant handle functional loads.
Some surface technologies incorporate calcium phosphate or hydroxyapatite-like layers, which can be more directly bioactive by providing a chemistry similar to mineralised bone. These approaches may support bone bonding and early healing, but they also require durable coatings and consistent manufacturing to avoid long-term delamination risks. Importantly, no surface can compensate for poor surgical planning, uncontrolled bite forces, or inadequate oral hygiene; surface engineering is only one part of the biomechanical and biological system.
For screwless restorations specifically, strong osseointegration provides the stable foundation that allows the prosthetic connection to do its job. If the implant is not well integrated, any prosthetic joint—screw-retained, cemented, or friction-fit—will be exposed to higher micro-movement and more complex load patterns. In other words, surface design supports the “base layer” stability, while taper and press-fit engineering support the “top layer” retention and precision.
In summary, screwless dental implant restorations rely on tightly controlled mechanical principles: taper geometry and friction to resist separation, press-fit tolerances to prevent micro-movement and rotation, and implant surface engineering to promote reliable osseointegration. These innovations can improve aesthetics and simplify some aspects of the visible restoration, but they also place high demands on precision, cleanliness of the interface, and planned maintenance so that stability and retrievability remain predictable over time.




