Overview of Sperm Donation Centers
Navigating sperm donation in the United States involves understanding unique processes, legal frameworks, and diverse donor criteria. From growing demand among LGBTQ+ families to the rise of at-home kits and changing regulations, explore what’s shaping American sperm banks in 2026.
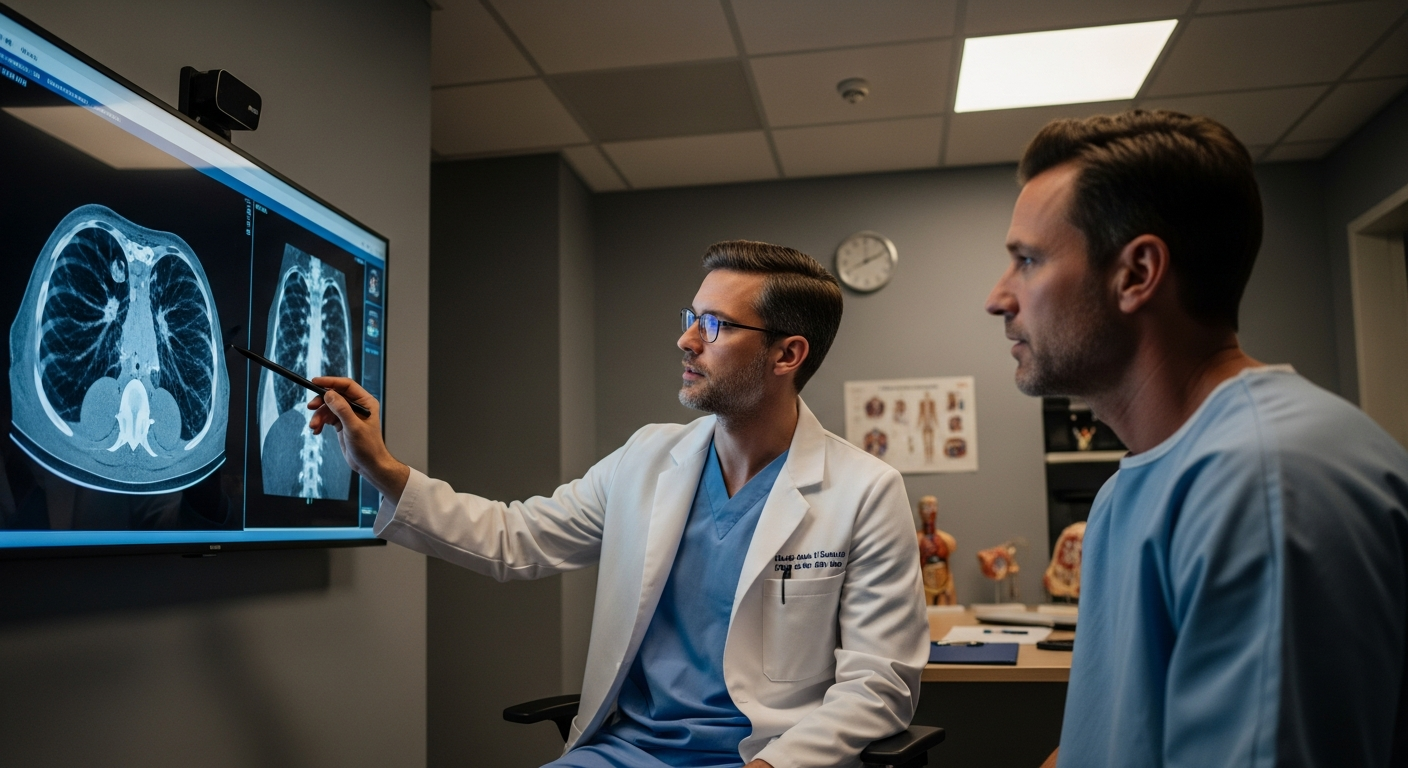
Across the United States, reproductive tissue banks and fertility clinics help people pursue parenthood through regulated screening, laboratory handling, storage, and distribution of donor samples. These organizations operate at the intersection of medicine, family law, and personal decision-making, so their processes are often more detailed than many people expect. For intended parents, donors, and donor-conceived families, understanding the system can make terminology, timelines, and responsibilities much clearer.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
How U.S. centers typically operate
Most U.S. centers begin with donor recruitment, medical intake, and preliminary eligibility checks. If an applicant meets initial requirements, the center moves to laboratory testing, detailed questionnaires, and counseling or education about the donation process. Approved samples are collected, analyzed, frozen, quarantined when required, and stored in specialized facilities. Intended parents usually review donor profiles that may include health history, education, physical traits, and sometimes audio interviews, photos, or personal essays, depending on the center’s policies.
Centers must also follow a chain of documentation. Identity verification, consent forms, infectious disease screening, and record retention are central parts of routine operations. In the United States, the Food and Drug Administration regulates human cells and tissue products, and professional groups such as the American Society for Reproductive Medicine provide additional practice guidance. While standards are broadly shared, the exact process can vary between large national cryobanks, hospital-based fertility programs, and smaller local services in your area.
Donor eligibility and screening
Donor eligibility standards are designed to reduce medical risk and improve transparency. Screening often includes infectious disease testing, semen analysis, genetic carrier screening, family medical history review, and an assessment of lifestyle factors that may affect suitability. Many centers also use age limits and exclude applicants with certain health histories, high-risk exposures, or incomplete family background information. Psychological screening may be used as well, especially when identity-release programs are offered.
The goal is not simply to approve as many donors as possible. A reliable center is expected to apply consistent laboratory protocols and clear medical criteria before a sample is ever made available. For intended parents, this is one reason profiles may seem selective or limited. Screening standards can differ in depth, but reputable programs usually explain what was tested, what was self-reported, and what cannot be guaranteed, including future health outcomes or genetic developments that were unknown at the time of donation.
Legal issues and donor rights
Legal Considerations and Donor Rights are among the most important parts of this subject because laws are not fully uniform across the country. Contracts typically address consent, storage, use of samples, identity disclosure policies, and the intended legal relationship between donor and recipient family. In many clinic-based arrangements, the donor does not assume parental rights or obligations, but the legal framework depends on state law, the form of conception, and whether procedures were handled through licensed medical channels.
Privacy rules also matter. Some programs offer anonymous donation, while others emphasize open-identity or identity-release arrangements that may allow a donor-conceived adult to request identifying information later. Recordkeeping, future contact expectations, and the handling of medical updates should be understood before any agreement is signed. Because legal outcomes can differ by jurisdiction, families and donors often benefit from legal advice specific to their state rather than relying on assumptions based on another clinic or another region.
Family building and broader access
The Rise of LGBTQ+ and Single-Parent Families has shaped how many centers present services and support materials. More clinics now design intake forms, counseling options, and profile systems for a broader range of households, including single mothers by choice, same-sex couples, transgender and nonbinary patients, and families using reciprocal or collaborative reproductive plans. This shift has encouraged more inclusive language and more flexible approaches to donor matching, family goals, and future disclosure to children.
At the same time, broader access raises practical questions. Families may compare open-identity options, sibling limits, shipping logistics, and long-term record access differently depending on their structure and location. Counseling is often recommended because donor conception can involve emotional, ethical, and identity-related decisions that continue well beyond treatment. Centers that acknowledge these realities tend to provide more useful educational support than those that focus only on laboratory logistics.
Examples of established U.S. providers
Several well-known U.S. organizations illustrate how the field is structured, though their policies, donor availability, and profile access can differ.
| Provider Name | Services Offered | Key Features/Benefits |
|---|---|---|
| California Cryobank | Donor screening, storage, profile access, shipping | Large national presence, extensive donor profiles, long-established operations |
| Fairfax Cryobank | Donor screening, genetic testing options, storage, distribution | Broad donor catalog, multiple specimen options, educational resources |
| Seattle Sperm Bank | Donor matching, screening, specimen storage, shipping | Strong digital profile access, family-oriented educational materials |
For intended parents, comparing providers often involves more than catalog size. Important differences may include identity-release policies, medical updates, staff support, storage practices, family limits, and how clearly screening information is explained. A larger provider may offer wider geographic reach, while a smaller clinic may provide more individualized communication through local services.
Technology and at-home collection
Advances in Technology and At-Home Donation Kits have changed expectations around convenience, but they have not removed the need for medical oversight. Digital profile systems, expanded genetic testing, and improved cryostorage methods have made donor information easier to review and samples easier to transport. Some companies also market home collection or mail-in options for certain parts of the process, which may appeal to people seeking privacy or a simpler first step.
Even so, at-home systems have limits. Collection quality, shipping conditions, documentation, and timing can affect whether a sample meets clinical standards. Home-based options also do not replace legal review, infectious disease screening requirements, or the broader counseling that many families need. Technology can improve access and efficiency, but the most reliable outcomes still depend on transparent policies, qualified laboratory handling, and careful alignment between medical practice and state law.
Taken together, U.S. donation centers are structured around screening, documentation, and long-term record management rather than simple sample collection. The most important differences between programs often involve legal clarity, medical testing, identity policies, and the quality of communication offered to donors and families. As technology expands and family structures continue to diversify, these centers are likely to remain an important part of reproductive care while balancing ethics, safety, and informed choice.




