Myelodysplastic Syndrome: Silent Signals You Shouldn’t Ignore
Could your body be revealing signs of a serious blood disorder without your awareness? Myelodysplastic syndrome (MDS) can develop quietly, with subtle signals that are easy to miss. In this article, we highlight the warning signs you shouldn’t overlook and explain why noticing them early can help you take informed steps toward better health.Myelodysplastic syndrome affects thousands of Americans each year, yet many people remain unfamiliar with this complex blood disorder. The condition occurs when the bone marrow, responsible for producing blood cells, begins creating abnormal or immature cells that cannot function properly. These defective cells accumulate in the bone marrow and bloodstream, leading to various health complications that can significantly impact quality of life.
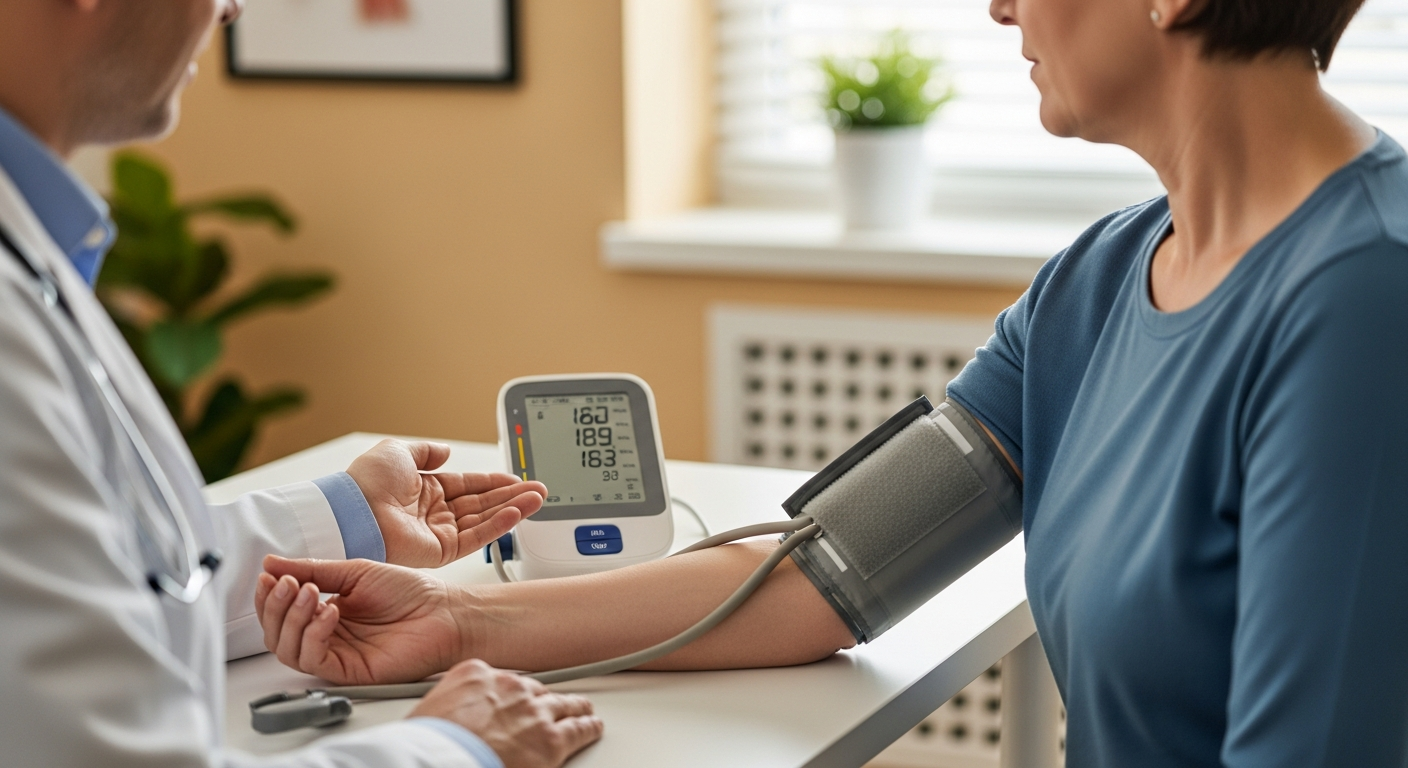
Changes in your energy, breathing, and resistance to infections can sometimes signal more than just a hectic schedule or getting older. Myelodysplastic syndrome (MDS) is a bone marrow disorder that often develops gradually, making its early symptoms easy to overlook. Understanding how it arises, who is more likely to develop it, and which warning signs to watch for can help you recognize when it may be time to ask a healthcare professional for a closer look.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
What is myelodysplastic syndrome and who is at risk?
Myelodysplastic syndrome is a group of conditions in which the bone marrow no longer produces blood cells normally. The marrow contains stem cells that should mature into healthy red blood cells, white blood cells, and platelets. In MDS, these stem cells develop abnormal changes, so many new blood cells die early or never fully mature. Even though the marrow may appear crowded, the bloodstream may still be low in one or more types of blood cells.
MDS is diagnosed more often in older adults, particularly those over 60. A history of chemotherapy or radiation for a different cancer can increase risk, because these treatments may damage the DNA of marrow cells. Long-term exposure to certain chemicals, such as benzene found in some industrial settings, heavy tobacco use, and some rare inherited blood or bone marrow disorders can also contribute. In many people, however, no specific cause is identified.
What are the early warning signs of MDS?
Early signs of MDS are often subtle and nonspecific. Because red blood cells carry oxygen throughout the body, a shortage can cause persistent tiredness that does not improve with rest. People may notice they become winded more easily when walking, climbing stairs, or doing routine chores. Weakness, lightheadedness, and a feeling of being “worn out” much of the time are common complaints.
Other early clues can include pale skin or pale inner eyelids and gums. When white blood cells are low, infections may occur more often or take longer to clear, even if they seem mild at first. Low platelets may lead to easy bruising, small red or purple spots under the skin called petechiae, or more frequent nosebleeds or gum bleeding. Menstrual bleeding may become heavier or last longer than usual.
These symptoms do not automatically mean someone has MDS. They can also be linked to iron deficiency, vitamin shortages, chronic kidney or heart disease, or other forms of anemia. Still, when they are new, persistent, or steadily worsening, they deserve careful evaluation rather than being dismissed.
Why do these symptoms often go unnoticed?
Many people live with the early stages of MDS without realizing something serious is happening. Fatigue and decreased stamina are easy to attribute to aging, weight changes, poor sleep, or stress. People may gradually adjust their daily activities, avoiding stairs or longer walks and believing these changes are simply part of getting older.
Infections or bouts of illness may seem like bad luck or the result of being around others who are sick. Bruises can be excused as minor injuries that were not noticed at the time. When symptoms come and go or do not feel severe, it is common to postpone seeing a healthcare professional.
Even in medical settings, the slow and subtle nature of MDS can make it difficult to recognize early. Because many conditions can cause low blood counts, it may take repeat blood tests, review of a blood smear, and sometimes a bone marrow biopsy to confirm MDS. If routine screening blood work is not done regularly, the disorder can remain hidden for a long time.
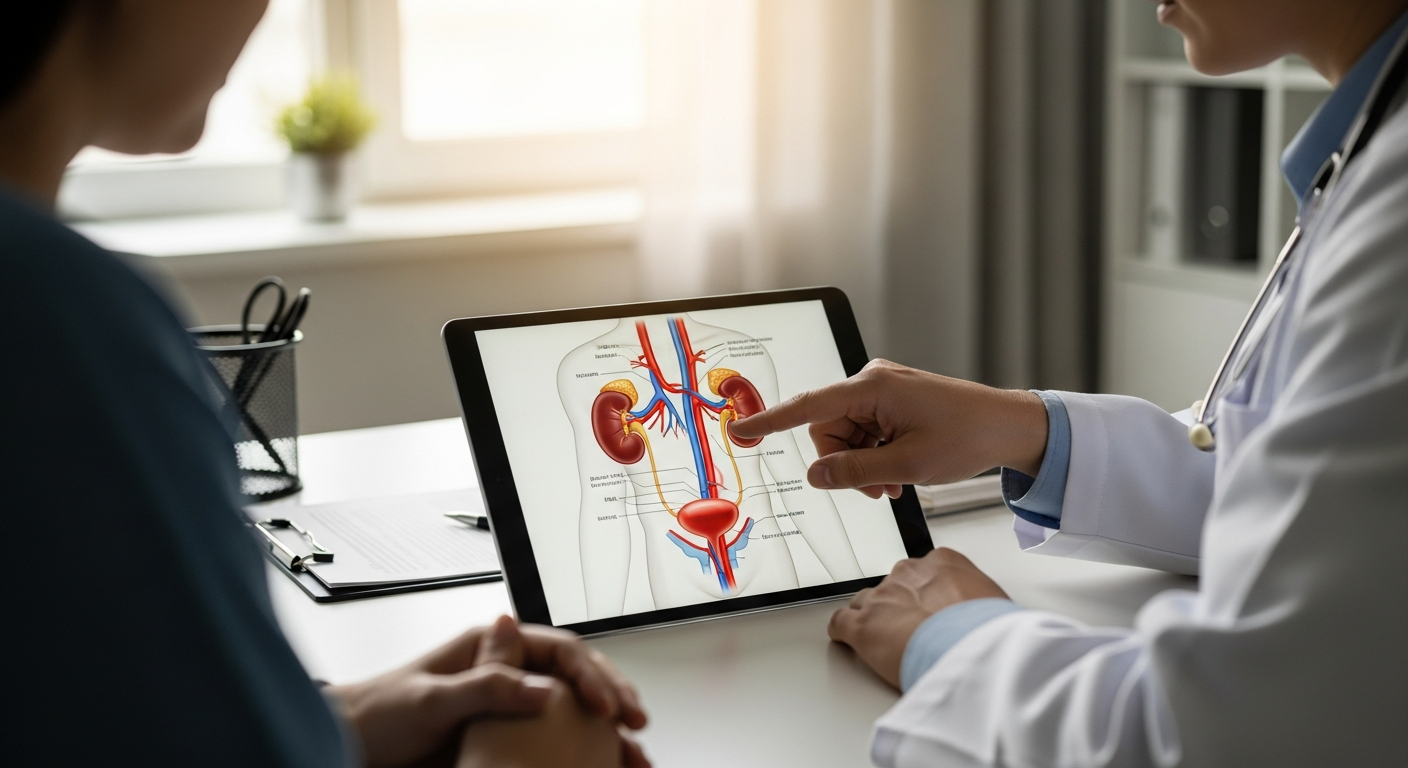
How does MDS affect your body’s blood production?
To understand why the symptoms appear, it helps to look more closely at normal blood production. In healthy bone marrow, stem cells divide and mature into three main blood cell types. Red blood cells carry oxygen; white blood cells help fight infection; and platelets are fragments that assist with clotting when you bleed.
In myelodysplastic syndrome, genetic changes inside the stem cells disrupt this process. The marrow may produce many immature or misshapen cells that are cleared away quickly because they cannot function properly. This leads to cytopenias, a medical term for low levels of one or more blood cell types in the circulation.
A shortage of red blood cells leads to anemia, causing fatigue, weakness, shortness of breath, and sometimes chest discomfort or rapid heartbeat. Low white blood cells, especially neutrophils, raise the risk of infections that may be more frequent, harder to treat, or recur after seeming to improve. A low platelet count can cause easy bruising, prolonged bleeding from small cuts, or spontaneous bleeding from the nose or gums. Over time, some cases of MDS may progress to a more aggressive blood cancer called acute myeloid leukemia, which requires urgent treatment.
When should you seek medical attention?
Knowing when to seek medical attention is an important part of responding to these silent signals. Persistent or unexplained fatigue that interferes with daily activities, especially if it is new or worsening, should prompt a conversation with a healthcare professional. The same is true for shortness of breath with mild exertion, such as walking a short distance or climbing a single flight of stairs.
Other reasons to seek evaluation include repeated infections, fevers without an obvious source, frequent or unusually large bruises, small red or purple spots on the skin, and bleeding from the nose or gums that seems out of proportion to any injury. People who have previously received chemotherapy or radiation, who have worked with certain industrial chemicals, or who have known blood or bone marrow disorders may wish to be especially alert to these signs.
A common first step in assessment is a complete blood count, a routine test that measures levels of red blood cells, white blood cells, and platelets. If blood counts are persistently low or appear abnormal, additional tests may be recommended, possibly including referral to a hematologist, a specialist in blood disorders. Even if MDS is not the cause, identifying the reason for ongoing symptoms can help prevent complications and support overall health.
By paying attention to changes in energy, breathing, bruising, and infections, it is possible to notice patterns that deserve professional attention. While myelodysplastic syndrome often develops quietly, recognizing these silent signals and discussing them with a trusted clinician can support earlier evaluation and more informed decisions about health and well-being.