Modern HIV Management: From Early Detection to Advanced Clinical Prevention Strategies
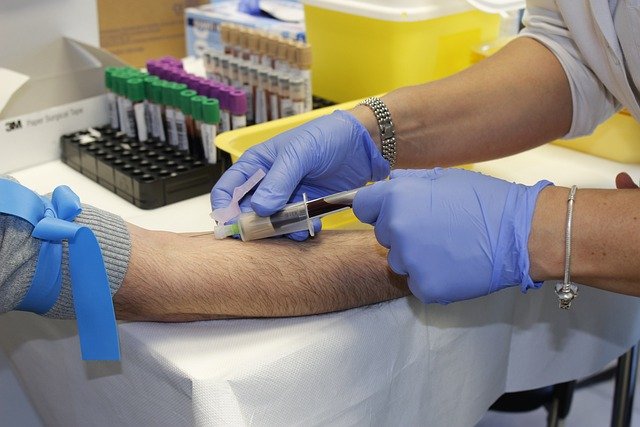
Modern advancements in medical science have fundamentally transformed the landscape of HIV care and prevention. Today, the focus has shifted from reactive measures to proactive strategies that prioritize long-term health and viral suppression. Understanding the available clinical pathways and preventive options is essential for individuals seeking to maintain their immune health and prevent transmission within their communities through informed medical decisions.
The landscape of HIV care has undergone remarkable transformation, shifting from reactive treatment models to comprehensive prevention and management frameworks. Modern clinical approaches integrate cutting-edge diagnostics, personalized therapeutic regimens, and preventive measures that significantly reduce transmission rates and improve quality of life for those living with the virus.
Transitioning from Observation to Proactive Biomedical Defense Protocols
Historically, HIV management focused primarily on treating symptoms as they emerged. Contemporary medicine has pivoted toward proactive intervention, emphasizing early detection through routine screening and immediate therapeutic engagement upon diagnosis. This shift recognizes that viral suppression achieved through early treatment not only preserves immune function but also prevents transmission to others. Healthcare systems now prioritize regular testing for at-risk populations, enabling clinicians to initiate antiretroviral therapy before significant immune system damage occurs. The concept of treatment as prevention has revolutionized public health strategies, with studies demonstrating that individuals maintaining undetectable viral loads cannot transmit the virus sexually.
Evaluating Modern Oral Prophylaxis for Daily Immune Protection
Pre-exposure prophylaxis, commonly known as PrEP, represents a groundbreaking advancement in HIV prevention. This daily oral medication regimen allows HIV-negative individuals at substantial risk to protect themselves from infection. The most widely prescribed formulations combine tenofovir with emtricitabine, creating a protective barrier when taken consistently. Clinical trials have shown effectiveness rates exceeding 90% among adherent users. Healthcare providers assess individual risk factors including sexual behavior patterns, partner status, and other considerations when determining candidacy for prophylactic therapy. Access has expanded significantly across the United States, with many insurance plans covering these medications and assistance programs available for eligible individuals. Regular monitoring through quarterly clinical visits ensures ongoing safety and effectiveness.
The Role of Genomic Diversity in Shaping Personalized Treatment Responses
HIV exhibits remarkable genetic variability, with multiple subtypes and recombinant forms circulating globally. This diversity influences how individuals respond to specific antiretroviral medications. Resistance testing has become standard practice, analyzing viral genetic sequences to identify mutations that may compromise drug effectiveness. Clinicians use these results to design personalized treatment regimens that account for both viral characteristics and patient-specific factors including other health conditions, potential drug interactions, and lifestyle considerations. Advances in pharmacogenomics further refine this approach, examining how individual genetic variations affect medication metabolism and response. This precision medicine framework maximizes therapeutic success while minimizing adverse effects, moving away from one-size-fits-all protocols toward tailored interventions.
Navigating Access to Preventive Therapy via Modern Clinical Enrollment
Despite significant therapeutic advances, accessing HIV prevention and treatment services remains challenging for many Americans. Multiple pathways exist for obtaining care, including community health centers, specialized HIV clinics, and primary care providers with infectious disease expertise. Federal programs such as the Ryan White HIV/AIDS Program provide comprehensive services for uninsured and underinsured individuals. Patient assistance programs offered by pharmaceutical manufacturers help eligible patients access medications at reduced or no cost. Telehealth has emerged as a valuable tool, particularly for individuals in rural areas or those facing transportation barriers, enabling remote consultations and prescription management. Community-based organizations play crucial roles in connecting individuals with clinical services, offering navigation support, and addressing social determinants that impact health outcomes. Understanding available resources and eligibility criteria empowers individuals to overcome access barriers.
Addressing Evolutionary Viral Adaptations through Precision Medical Consultation
HIV’s capacity for rapid mutation presents ongoing challenges in long-term management. The virus can develop resistance to antiretroviral medications, particularly when treatment adherence is inconsistent or drug levels remain suboptimal. Regular viral load monitoring detects treatment failure early, prompting timely regimen adjustments before extensive resistance develops. Specialists employ sophisticated strategies when resistance emerges, often combining newer medication classes or utilizing drugs with different resistance profiles. Integrase inhibitors, entry inhibitors, and newer formulations provide options when traditional therapies lose effectiveness. Consultation with infectious disease specialists becomes particularly important in complex cases involving multi-drug resistance or treatment-experienced patients. These experts stay current with emerging therapies and clinical trial opportunities, offering patients access to innovative approaches not yet widely available.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
Conclusion
Modern HIV management represents a remarkable achievement in medical science, transforming what was once a fatal diagnosis into a manageable chronic condition. The integration of early detection, personalized antiretroviral therapy, preventive medications, and comprehensive support services has dramatically improved outcomes for millions. As research continues advancing and access expands, the goal of ending the HIV epidemic becomes increasingly achievable. Individuals concerned about HIV exposure or living with the virus should engage with healthcare providers to explore the full range of available options tailored to their specific circumstances.