2026 Cataract Surgery: An Overview of the Latest Developments
With cataracts affecting millions of Americans, 2026 brings groundbreaking advances in surgery, from laser precision to AI-assisted diagnostics. Discover how shorter recovery times, improved insurance options, and expanded access are transforming cataract care across the United States.
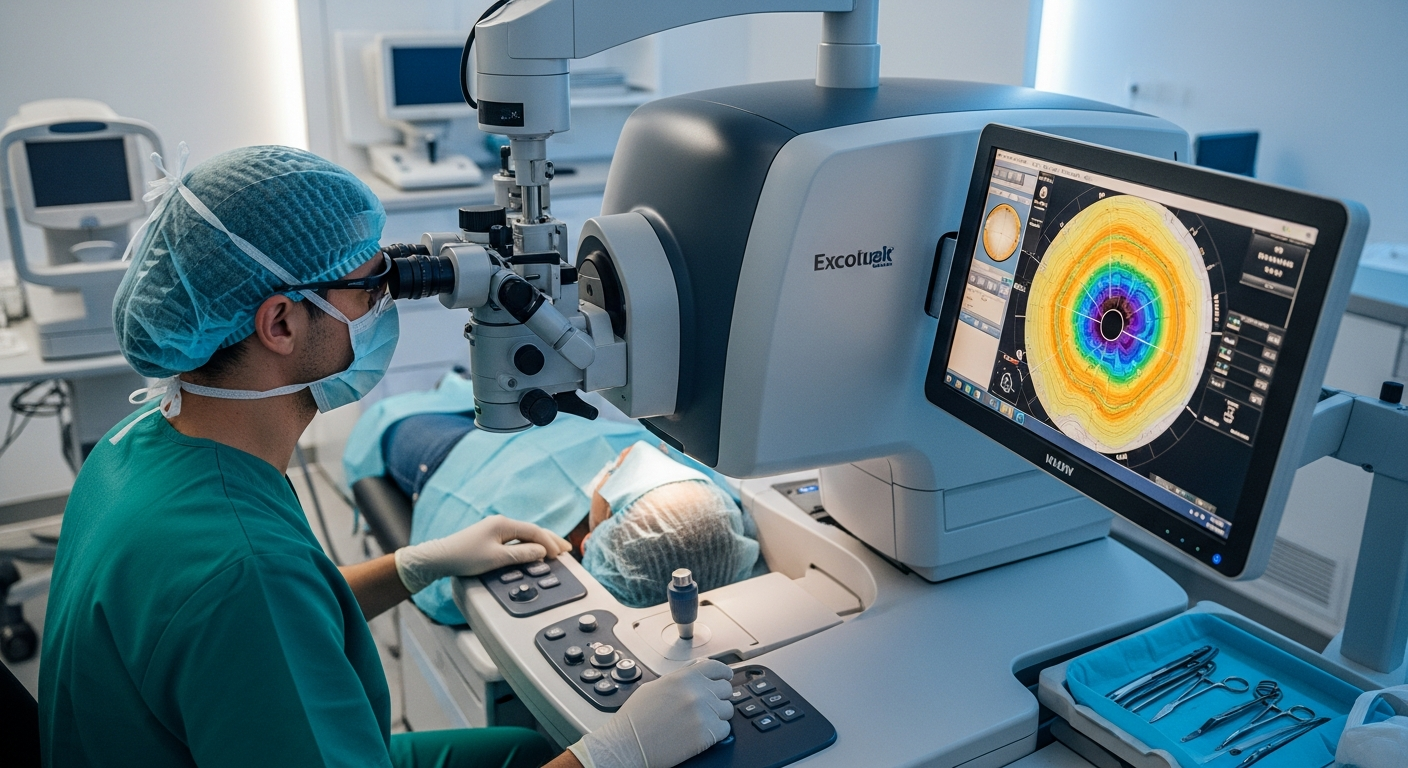
Modern lens-replacement surgery is among the most commonly performed outpatient procedures in the United States, and its steady refinement is shaped by better diagnostics, more customizable implants, and a growing emphasis on patient-centered care. Even with these advances, outcomes still depend on individual eye health, coexisting conditions, and practical factors like insurance rules and access to specialty care.
What’s new in cataract surgery technology?
Advances in Cataract Surgery Technology are often most visible before the first incision: diagnostics and planning have become more data-driven. Optical biometry, corneal topography, and wavefront-style measurements help surgeons estimate implant power and understand astigmatism with greater precision. Many practices also use digital planning tools that integrate measurements into surgical workflow, aiming to reduce manual transcription steps that can introduce avoidable errors.
Inside the operating room, techniques continue to emphasize small-incision approaches, stable fluidics, and efficient removal of the clouded lens. Femtosecond laser–assisted steps may be available in some centers for portions of the procedure (such as creating corneal incisions or fragmenting the lens), although use varies and not every patient is a candidate. Newer intraocular lens (IOL) options—including toric lenses for astigmatism and presbyopia-correcting designs—offer more ways to tailor vision goals, but they can involve trade-offs like glare, halos, or reduced contrast sensitivity for certain people.
What can patients expect during recovery?
Patient Experience and Post-Op Recovery typically look different now than they did decades ago, largely because the procedure is usually quick, uses a tiny incision, and is commonly performed under local anesthesia with light sedation. Many patients notice vision improving within days, but it can take longer for the eye to fully stabilize—especially if the surface of the eye is dry, if there is pre-existing astigmatism, or if both eyes are treated on separate dates.
A realistic recovery plan includes more than “time.” Post-op care often involves prescription eye drops (or, in some cases, alternative medication delivery approaches selected by the surgeon), temporary activity adjustments, and follow-up visits to confirm that the implant is well positioned and that eye pressure and inflammation are controlled. People with diabetes, glaucoma, macular degeneration, significant dry eye, or a history of eye surgery may need closer monitoring, because those conditions can affect both healing and final visual quality.
How are eye care disparities being addressed?
Addressing Health Disparities in Eye Care has become a more explicit focus as health systems and public agencies recognize that preventable vision impairment is not distributed evenly. In practice, disparities can stem from cost-sharing burdens, limited transportation, fewer nearby specialists, lack of paid time off, language barriers, and differences in the timing of referrals. These barriers can lead to delayed evaluation, reduced follow-up, or lower uptake of recommended treatment.
Efforts that can help include community-based screening programs, clearer referral pathways from primary care and optometry to ophthalmology, expanded interpreter services, and telehealth-supported pre-visit education when appropriate. At the clinic level, simpler scheduling, transparent pre-op instructions, and support navigating coverage rules can reduce missed appointments. On a broader level, improving surgical access in underserved areas often depends on workforce distribution, facility availability, and insurance network adequacy—factors that can vary widely “in your area,” even within the same state.
How do insurance coverage and costs work in the U.S.?
Insurance Coverage and Costs in the U.S. can be confusing because the total price includes multiple components (surgeon fee, facility fee, anesthesia services, diagnostic testing, and the lens implant), and coverage depends on the payer and the choices made for lens type and technique. In general, standard surgery with a conventional monofocal lens is more likely to be covered under major plans when medically necessary, while upgrades such as presbyopia-correcting lenses, some astigmatism-correcting options, or laser-assisted steps may involve added out-of-pocket costs. The comparison below summarizes common real-world structures used by major U.S. payers and plan types; exact benefits still depend on the specific policy and whether clinicians and facilities are in-network.
| Product/Service | Provider | Cost Estimation |
|---|---|---|
| Standard surgery with monofocal IOL (facility + surgeon) | Medicare Part B (typical coverage model) | Patient responsibility commonly includes deductible and coinsurance; exact allowed amounts vary by region and setting |
| Standard surgery with monofocal IOL (in-network) | Blue Cross Blue Shield (plan-dependent) | Often subject to deductible, copay/coinsurance; out-of-network care may cost more |
| Standard surgery with monofocal IOL (in-network) | UnitedHealthcare (plan-dependent) | Typically deductible plus coinsurance/copay; prior authorization rules may apply |
| Standard surgery with monofocal IOL (in-network) | Aetna (plan-dependent) | Commonly deductible plus copay/coinsurance; coverage varies by employer/marketplace plan |
| Elective “premium” upgrades (e.g., presbyopia-correcting IOLs, some laser-assisted fees) | Many commercial insurers and Medicare (coverage often limited) | Frequently involves additional out-of-pocket charges; typical market benchmarks can range from hundreds to several thousand dollars per eye depending on selections and location |
Prices, rates, or cost estimates mentioned in this article are based on the latest available information but may change over time. Independent research is advised before making financial decisions.
In day-to-day budgeting, patients often find it useful to request an itemized estimate that separates medical benefits (what insurance may cover) from elective upgrades (what may be self-pay). It also helps to ask whether the surgery is scheduled at a hospital outpatient department or an ambulatory surgery center, because contracted rates and patient cost-sharing can differ. Prescription eye drops, post-op visits, and treatment of dry eye may add incremental costs that are easy to overlook if the focus stays only on the procedure itself.
What future trends are shaping research and treatment?
Future Trends and Research in Cataract Treatment are increasingly tied to personalization and safety. Research continues on new IOL materials and designs intended to balance range of vision with fewer night-vision side effects, as well as improved methods to measure and manage ocular surface disease before surgery (since dry eye can distort measurements and reduce satisfaction). There is also ongoing interest in using data analytics to refine IOL power calculations for patients with prior refractive surgery or atypical eye anatomy—groups where lens calculations can be more challenging.
Another likely direction is more integrated care pathways: streamlined pre-op workups, clearer expectation-setting tools, and post-op monitoring that prioritizes early detection of complications such as infection, inflammation spikes, pressure changes, or macular swelling. While many innovations can improve consistency, it remains important to treat technology as one part of the outcome equation—alongside surgical skill, careful patient selection, and adherence to follow-up.
Overall, today’s approach emphasizes precise measurement, thoughtful lens selection, and recovery planning that accounts for each person’s broader eye health and daily needs. Cost and access remain central issues in the United States, making transparency and equitable pathways to specialty care as important as technical progress. This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.