Early Signs of HIV You Should Never Ignore
Early detection of HIV can make a huge difference in treatment and quality of life. Recognizing warning signs such as unexplained fatigue, fever, swollen lymph nodes, and unusual infections is crucial. Learn the early indicators, risk factors, and when to seek medical advice to protect your health.
Human Immunodeficiency Virus remains a significant public health concern in the United States, affecting approximately 1.2 million people. While modern treatments have transformed HIV from a fatal diagnosis to a manageable chronic condition, early detection remains critical. Many people experience symptoms within the first few weeks of infection, yet these signs are often overlooked or attributed to other causes. Understanding these early warning signs and taking prompt action can make a substantial difference in long-term health outcomes.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
What Is HIV and How It Affects the Body
HIV is a virus that attacks the immune system, specifically targeting CD4 cells, which are white blood cells that help the body fight infections. When HIV enters the body, it begins replicating rapidly, using these immune cells as hosts. As the virus multiplies, it gradually weakens the immune system’s ability to defend against diseases and infections. Without treatment, HIV can progress to AIDS (Acquired Immunodeficiency Syndrome), the most advanced stage of infection. The virus is transmitted through contact with certain bodily fluids, including blood, semen, vaginal fluids, rectal fluids, and breast milk. Modern antiretroviral therapy can reduce the viral load to undetectable levels, preventing transmission and allowing people with HIV to live long, healthy lives. Understanding how HIV operates helps explain why early symptoms occur and why prompt testing matters.
Common Early Symptoms
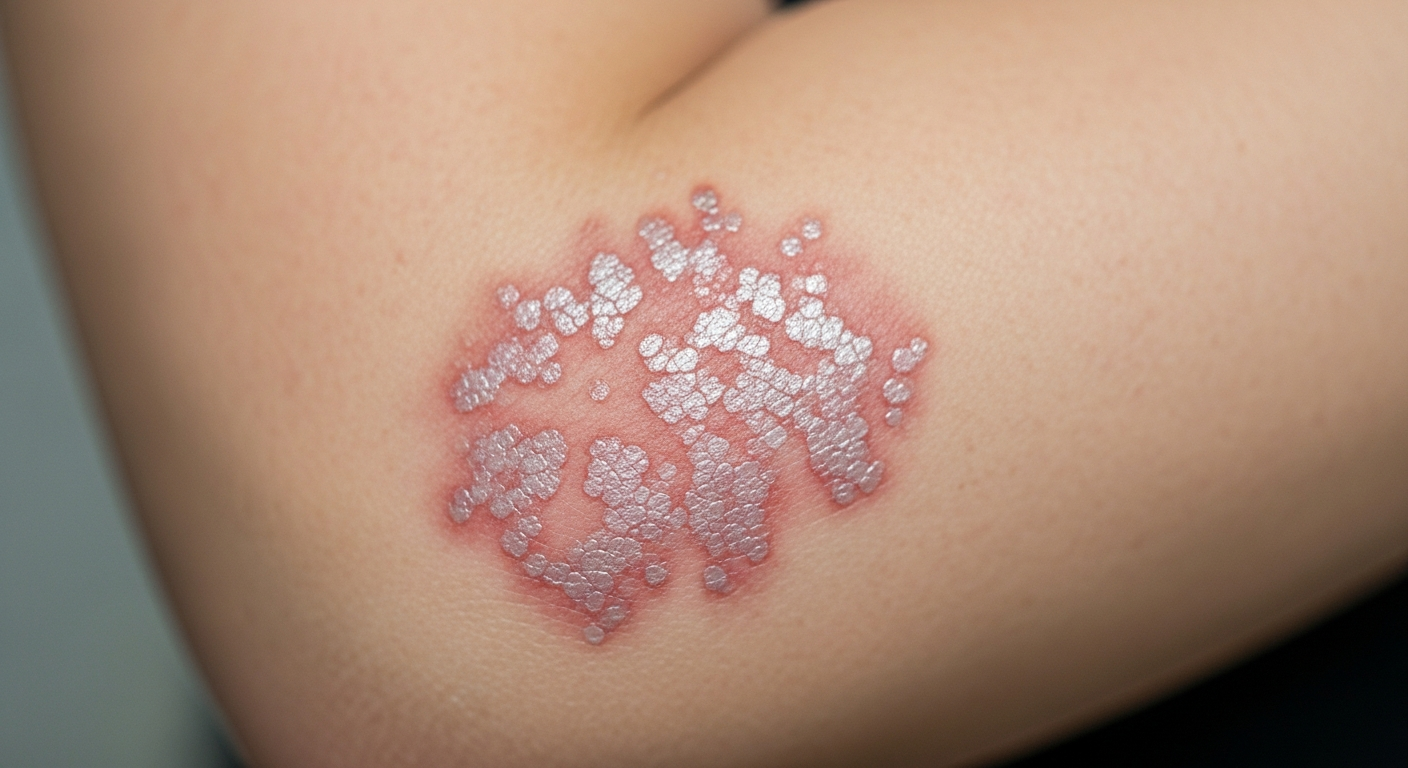
The initial phase of HIV infection, known as acute HIV infection or acute retroviral syndrome, typically occurs two to four weeks after exposure. During this period, the virus is multiplying rapidly, and the body’s immune response triggers flu-like symptoms. Common early signs include persistent fever, often accompanied by chills and night sweats. Many people experience severe fatigue that interferes with daily activities, along with swollen lymph nodes in the neck, armpits, or groin. A sore throat, muscle aches, and joint pain are frequently reported. Some individuals develop a rash, typically appearing on the torso, face, or extremities, characterized by small red bumps or patches. Headaches, mouth ulcers, and digestive issues such as nausea, vomiting, or diarrhea may also occur. These symptoms can last from a few days to several weeks. Because they resemble common viral infections like the flu or mononucleosis, many people do not immediately recognize them as potential HIV symptoms. However, if you have recently engaged in activities that could expose you to HIV and experience these symptoms, testing is essential.
Risk Factors and Who Is Most Vulnerable
Certain behaviors and circumstances increase the likelihood of HIV transmission. Unprotected sexual contact, particularly receptive anal intercourse, carries the highest risk. Having multiple sexual partners or a partner with HIV also increases vulnerability. Sharing needles or syringes for drug use is another major transmission route. Healthcare workers who experience needle-stick injuries face occupational risk, though this is relatively rare with proper safety protocols. People with other sexually transmitted infections are more susceptible to HIV because these infections can create breaks in the skin or mucous membranes. Infants born to mothers with HIV can acquire the virus during pregnancy, childbirth, or breastfeeding, though transmission can be prevented with appropriate medical care. Certain populations experience disproportionately higher rates of HIV infection in the United States, including men who have sex with men, African American and Hispanic communities, and transgender individuals. Geographic location also plays a role, with higher infection rates in the Southern United States. Understanding these risk factors helps individuals assess their own vulnerability and make informed decisions about prevention and testing.
When and How to Get Tested
Testing is the only way to know your HIV status with certainty. The Centers for Disease Control and Prevention recommends that everyone between ages 13 and 64 get tested at least once as part of routine healthcare. Those with higher risk factors should test more frequently, potentially every three to six months. If you have experienced potential exposure to HIV, timing your test is important. Most modern tests can detect HIV within 18 to 45 days after infection, though some newer tests can identify the virus as early as 10 to 14 days. Testing during the window period, before antibodies or antigens reach detectable levels, may produce false negatives, so retesting may be necessary. Several testing options are available in the United States. Rapid tests provide results in 20 to 30 minutes and can be performed at clinics, community health centers, or at home using FDA-approved kits. Laboratory-based tests analyze blood samples and typically provide results within a few days. Combination tests detect both HIV antibodies and antigens, offering earlier detection than antibody-only tests. Many testing locations offer services on a confidential or anonymous basis, and numerous community organizations provide free testing. If you test positive, immediate connection to healthcare services ensures you can begin treatment promptly.
Interpreting Results and Next Steps
Receiving your test results can be emotionally challenging, regardless of the outcome. A negative result means no HIV infection was detected at the time of testing. However, if you tested during the window period or have had recent potential exposure, follow-up testing is recommended. Continue practicing prevention methods, including condom use and, if appropriate, pre-exposure prophylaxis (PrEP), a medication that significantly reduces HIV transmission risk. A positive result indicates HIV infection and requires immediate medical attention, but it is not a death sentence. Modern antiretroviral therapy is highly effective, and many people with HIV achieve undetectable viral loads, meaning they cannot transmit the virus to others. After a positive diagnosis, healthcare providers will conduct additional tests to measure viral load and CD4 cell count, which help determine the stage of infection and guide treatment decisions. Starting treatment as soon as possible preserves immune function and prevents progression to AIDS. Your healthcare team will help you navigate treatment options, manage potential side effects, and connect you with support services. Disclosure to sexual partners is important for their health and is legally required in some states. Many communities offer support groups, counseling services, and resources specifically for people living with HIV. With proper medical care and adherence to treatment, people with HIV can live long, fulfilling lives with near-normal life expectancy.
Recognizing early HIV symptoms and seeking prompt testing can dramatically improve health outcomes. While the initial signs may seem minor or easily dismissed, they represent a critical window for intervention. Understanding how HIV affects the body, knowing your risk factors, and accessing appropriate testing services empowers you to take control of your health. Whether your results are positive or negative, knowledge of your status allows you to make informed decisions about treatment, prevention, and protecting others. The landscape of HIV care has transformed dramatically over recent decades, offering hope and effective management options that were once unimaginable.




